Devices
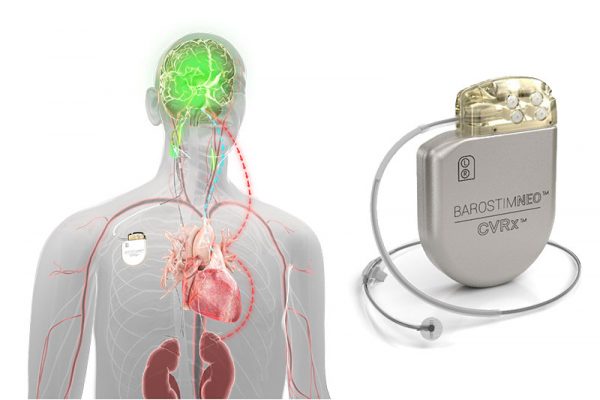
Unlike vagal stimulation, this therapy targets the afferent as well as the efferent different neural pathways and it restores the balance of sympathetic and vagal systems. Thereby, a causes vasodilation in the peripheral vasculature, decreasing the afterload, improve forward cardiac output, and functionality. BAROSTIM therapy also reduces heart rate because of the vagal activity. In general, you can expect the six-minute walk test to increase, quality of life to improve, functional class improvement, and reduction in BNP. There are no mortality days at this time.

A biventricular ICD a small device used for cardiac resynchronization therapy for patients with heart failure. This constantly monitors your heart rate and rhythm and delivers small electrical impulses to both the left and right ventricles to help them contract at the same time.

A biventricular pacemaker a small device used for cardiac resynchronization therapy for patients with heart failure. This delivers small electrical impulses to both the left and right ventricles to help them contract at the same time. This helps the heart to pump blood more efficiently with each beat.

The CardioMEMS™ HF System uses a miniaturized, wireless monitoring sensor that is implanted in the pulmonary artery during a minimally invasive procedure to directly measure PA pressure.
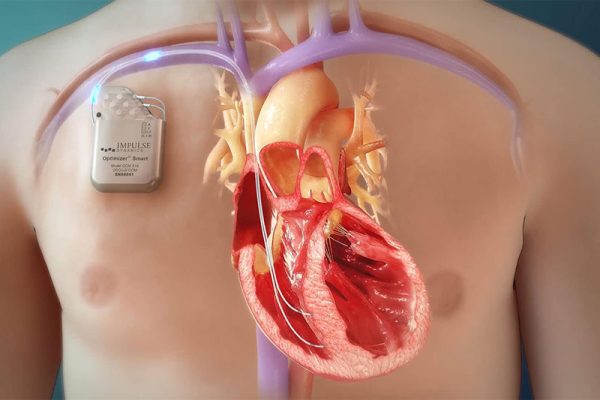
The Optimizer Smart system is an implantable device like a pacemaker that delivers Cardiac Contractility Modulation (CCM) therapy. This is a new therapeutic approach to manage symptoms or slow the progression of heart failure that improves quality of life for patients that are no longer adequately responding to medications intended.

The FreeStyle Libre Pro sensor continually measures and stores your sugar levels for up to 14 days. After you’ve worn the sensor for up to 14 days, your doctor will download data from it that will give information about how your sugar levels are trending throughout the day and night. This will help your doctor personalize your treatment plan.

A cardiac event monitor is a small portable device worn by patients during their normal activity for up to 30 days. This device is capable of recording the electrical activity of the heart in the form of an electrocardiogram (EKG) for up to several minutes. This is intended to record arrhythmias (abnormal heart rhythm) that would not be found on a routine EKG or to record an arrhythmia that is so infrequent, it is not detected on a 24 hour Holter monitor.
A Holter monitor is a small portable device used to record the electrical activity of the heart. A Holter monitor is typically worn for 24 hours to record each heart beat during your normal daily activity. This is performed to detect any irregular heart rhythms that may not be picked up on a routine electrocardiogram (EKG) during your office visit.

An ICD is a small device that monitors the electrical activity of the heart. This not only evaluates the hearts activity, but can also store the electrical events so Dr. Jamnadas can assess them. In the event a dangerously fast heart rhythm is detected, the ICD quickly delivers therapy in the form of electrical energy. This helps to regulate a normal heart rate and rhythm.

