What is Renal Artery Stenosis?
Renal artery stenosis is a narrowing in the artery that supplies the kidney with blood. Therefore the kidney senses low perfusion pressure and assumes that the body has low blood pressure, and produces chemicals that raise blood pressure. The patient subsequently experiences high blood pressure or hypertension. The stenosis is usually at the origin of the renal artery and occurs predominantly in elderly patients who have atherosclerosis and vascular disease elsewhere also. They are usually on multiple antihypertensive medications.
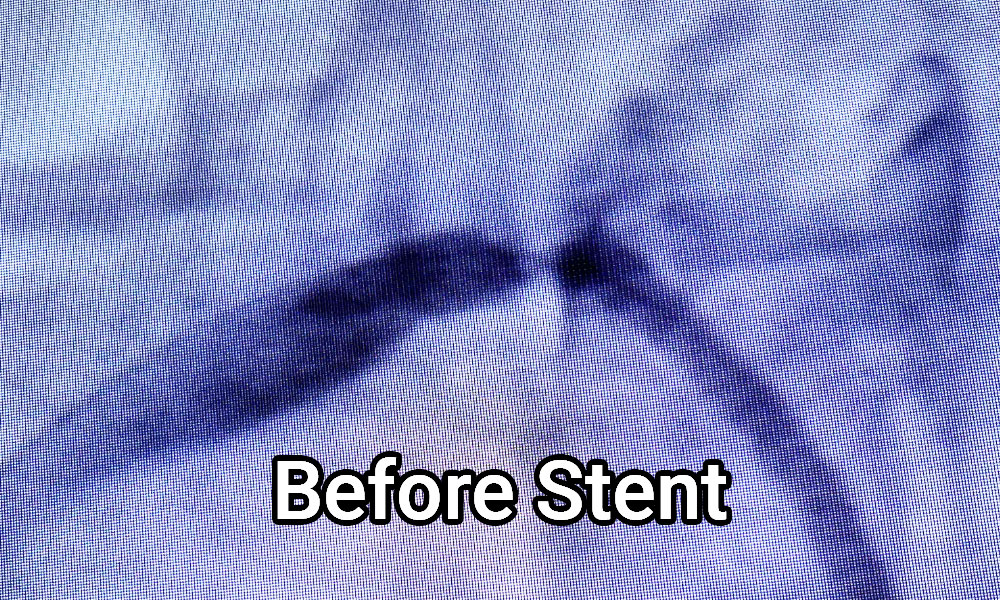
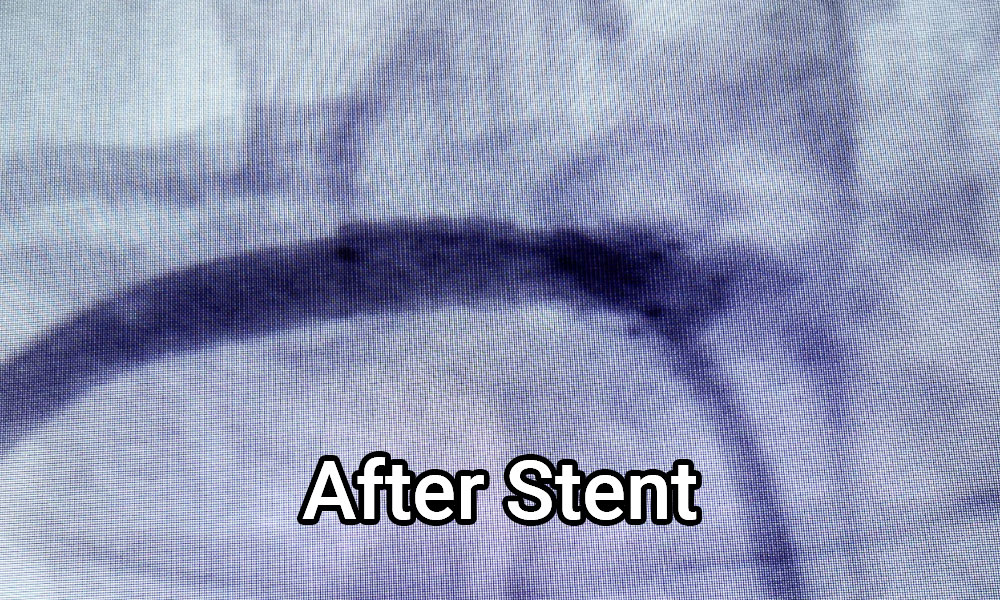
In the before picture, a tight stenosis is noted at the origin of the right renal artery, and after the stent placement, it is eradicated. Greater than 50% of the times, the patient is able to substantially reduce antihypertensive medication use or eliminate them completely. The procedure is used selectively because if the patient really has intrinsic renal disease or other causes of hypertension, then, a stent to the renal artery may not result in drastic reductions in blood pressure.
What are the causes?
- Fibromuscular dysplasia (narrowing due to thickening of internal wall of blood vessel) tends to run in families and is seen more in women below the age of 50. This usually involves the distal portion of the renal artery.
- Inflammation of the arteries known as arteritis may cause narrowing.
How does it occur?
A blockage of 50-70% of the renal artery is considered significant. As a result of decreased blood flow to the kidneys, the kidney cells falsely presume that blood flow throughout the entire body is reduced.
As a normal defense mechanism, the kidney activates a hormonal system known as the renin-angiotensin system. This response expands blood volume and elevates blood pressure throughout the entire body.
What are the risk factors?
- Men have a higher incidence compared to women
- Increasing age
- Family history of cardiovascular disease
- Smoking
- Excessive alcohol intake
- Diabetes
- High blood pressure
- Chronic Inflammation: i.e. viral infections
- Increased cholesterol levels
- Compression from a mass
What are the symptoms?
- Above the age of 50 or below the age of 30 with high blood pressure
- Who have had the need for more than 5 medications including a diuretic to control blood pressure
- Whose previously controlled blood pressure becomes uncontrollable
- With aortic or extensive peripheral vascular disease
- With worsening renal function
- With asymmetrical kidney sizes
- With flash pulmonary edema
What are the complications?
- Aortic Aneurysm
- Heart attack
- Congestive heart failure
- Kidney failure
- Stroke
How is it diagnosed?
- Patient History:
- Physical Examination:
- Testing
Laboratory investigations:
- Blood Analysis– this includes a complete blood count (CBC), electrolytes, renal function tests (urea and creatinine).
- Urine Analysis– to search for the presence of any blood in the urine.
Imaging Studies:
- Renal Ultrasound or Doppler– is a simple office procedure done to screen renal artery stenosis in high risk patients. The advantage of this test is that it is able to measure the size of a narrowing and measure the blood flow through the vessel.
- Renal Angiography– is the definitive diagnosis of renal artery stenosis. This is an invasive test done in a hospital setting, involving the insertion of a thin catheter into the groin, which passes through the aorta, then is advanced to the renal arteries. A contrast dye is given to view the arteries which are seen under x-ray guidance. This shows the exact number, location, and size of blockages. The advantage of an angiography is if a significant blockage is discovered, angioplasty or stenting may be done at the same time.
- Magnetic Resonance Angiography (MRA) – this is a test similar to an MRI, which involves a contrast dye to be injected into a vein, while pictures are taken of the renal arteries.
- Computed Tomographic (CT) Angiography: this test also involves the injection of a dye into the vein while pictures of the renal arteries are taken.
How is it treated?
- First line of treatment is to reduce the risk factors by diet changes, exercise, and weight management.
- Eat foods high in fiber such as whole grain cereals, oatmeal, and figs. Eat plenty of fruits such as apples, bananas, prunes, oranges, and pears. Include fish and legumes such as beans or chickpeas.
- Lower your salt intake
- Avoid fatty foods including bad saturated fat that is found in some meats, dairy products, chocolates, baked goods, and deep-fried food.
- Maintain a healthy weight with a BMI below 25
- No smoking
- Limit alcohol to one glass a day if you chose to drink
- Be more physically active
- Relax and reduce stress
- Angiotensin Converting Enzyme (ACE) Inhibitors: lower blood pressure by preventing some of your natural chemicals to be made, promoting relaxation of the blood vessels and dilatation.
- Angiotensin II Receptor Blockers (ARBs): block the action of the natural chemicals that narrow blood vessels.
- Diuretics: sometimes referred to as “water pills”. These reduce sodium and water which lower blood volume. These drugs may cause worsening of renal function. Medications and renal function will need to be closely monitored.
- Calcium Channel Blockers: helps to relax the muscles surrounding the arteries, increasing blood flow, and lowering blood pressure.
- Cholesterol-lowering medications– these reduce cholesterol levels in those with conditions with atherosclerosis.
- Renal Angioplasty and stenting: Renal artery stenting is the preferred method of treatment of renal artery stenosis. A bare metal stent is placed inside the renal artery to restore the blood flow. Once normal blood flow is restored, the kidney stops producing hormones that cause hypertension. The re-narrowing rate following renal artery stenting is 20%. Many patients are able to decrease their blood pressure medication usage or even stop them completely after this procedure.
- Endarterectomy: is a procedure in which a catheter is used to scrape the inner lining of an artery. That material which is blocking the artery is extracted by the use of a catheter.
- Renal Artery Bypass: The area of blockage in a renal artery is bypassed by attaching a vessel used from another area, to a site proximal of the blockage and attaching the other end to an area beyond the blockage.
How can I prevent this?
- NO Smoking
- Limiting alcohol consumption
- Controlling high blood pressure, cholesterol, and diabetes
- Eating a healthy diet
- Keeping physically active with the right kind of exercise
- Maintain a healthy weight with a BMI <25
- Get an annual flu shot
- Reduce stress!